
<p>Granger Wootz/Getty Images</p>
As young adults transition from adolescence and take on more responsibility for their own health and well-being, accessible and affordable health care is critical for building a foundation for their long-term health in adulthood.
Yet young adults ages 19 to 25 have historically had the highest rates of uninsurance among all age groups, with about one in three young adults lacking insurance before the Affordable Care Act (ACA) was passed in 2010.
Many young adults in low-income households aged out of eligibility for public health insurance coverage through Medicaid or the Children’s Health Insurance Program (CHIP) before the ACA, and their employment patterns, such as their decreased likelihood of full-time employment, made them less likely than older adults to have an offer of employer-sponsored insurance coverage.
Coverage and access to care for young adults improved following the ACA, with specific improvements attributed to the dependent coverage provision.
To better understand how Medicaid expansion under the ACA affected young adults’ health care coverage, we conducted a new analysis examining trends between 2011 and 2018 in insurance coverage and access to care for young adults ages 19 to 25. We assessed the impact of Medicaid expansion on young adults by comparing changes in coverage and access measures in states that expanded Medicaid under the ACA with states that did not expand Medicaid. From our analysis, we found that Medicaid expansion significantly benefited young adults, especially young adults in low-income households.
Medicaid expansion increased coverage for all young adults, with larger improvements for those in low-income households
Between 2011 and 2018, uninsurance rates among young adults declined by 16.4 percentage points in states that expanded Medicaid and by 11.9 percentage points in nonexpansion states.
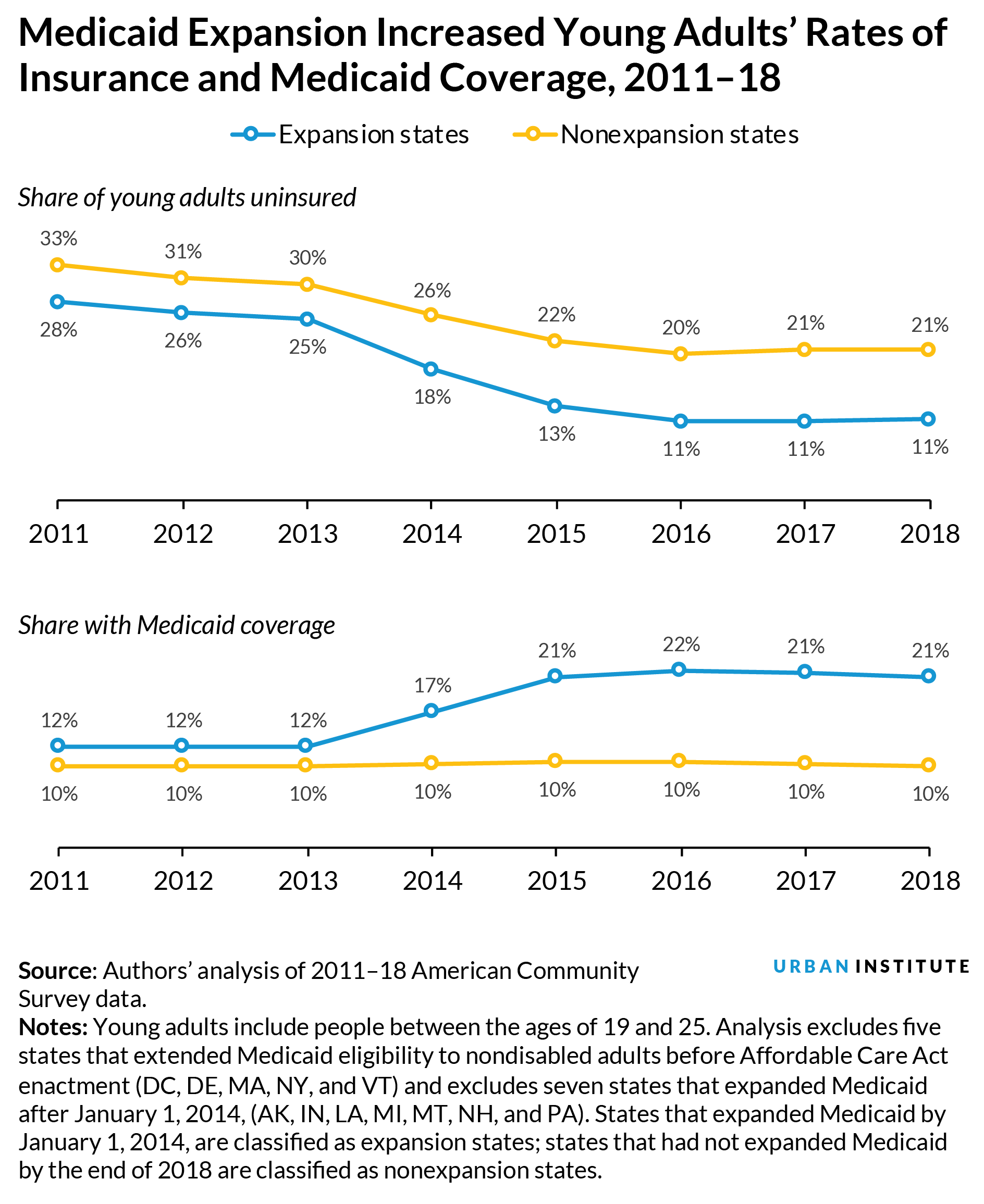
Among young adults in households with incomes below 200 percent of the federal poverty level, Medicaid expansion was associated with a 7.5 percentage-point decline in uninsurance rates relative to nonexpansion states.
Medicaid expansion was also associated with a 4.1 percentage-point increase in the likelihood of young adults in low-income households having a personal doctor.
Three policy solutions could further improve coverage and access to care
Although young adults’ health care coverage and access has increased following the ACA, many still lack access to quality health care. To ensure more young adults are covered, policymakers could pursue three policy solutions:
- Adopting ACA Medicaid expansion in the 12 remaining nonexpansion states could reduce uninsurance and increase access to care, particularly among young adults in low-income households or without a college degree. Recent analysis found that young adults would gain more coverage from Medicaid expansion in the remaining states than any other age group.
- Investing in outreach, such as increased marketing, targeted messaging to young adults, one-on-one enrollment assistance, and improved enrollment systems, could reduce uninsurance among young adults by enrolling those who are uninsured but eligible for Medicaid coverage.
- Expanding the availability of Marketplace premiums to young adults with incomes below the poverty level in nonexpansion states, increasing the value of Marketplace premium subsidies, and increasing cost-sharing reductions could reduce uninsurance among those not eligible for Medicaid coverage by increasing affordability of Marketplace coverage.
The effects of Medicaid expansion on young adult access and care measures provide evidence that further Medicaid expansions could improve overall health among young adults in low-income households throughout adulthood. But despite improved health insurance coverage rates, many young adults still went without preventive care in 2018. We find fewer than 60 percent of young adults received a checkup in the previous year or had a personal doctor, and only slightly more than one-quarter received a flu vaccine.
Policy efforts should ensure not only that young adults have health insurance coverage but also that insured young adults can afford to access and use the health care they need to build a foundation for their long-term health in adulthood.
Let’s help communities build more secure, hopeful futures.
Today’s complex challenges demand smarter solutions. Urban brings decades of expertise to understanding the forces shaping people’s lives and the systems that support them. With rigorous analysis and hands-on guidance, we help leaders across the country design, test, and scale solutions that build pathways for greater opportunity.
Your support makes this possible.