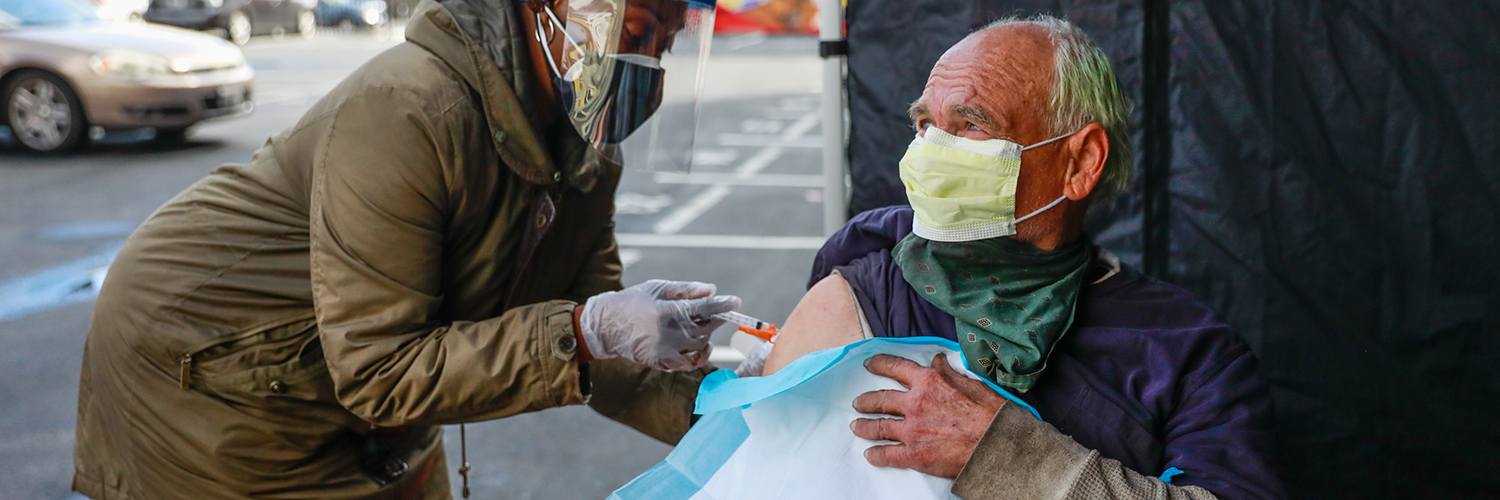
<p>Nurse Sonni Belcher-Collins (left) administers a dose of the Johnson & Johnson COVID-19 vaccine to Doug Rosen (right) on Thursday, March 11, 2021 in Oakland, California. The Trust Clinic hosted a mass vaccination day for people who are unhoused, housing insecure or staff members of the clinic. Gabrielle Lurie / The San Francisco Chronicle via Getty Images</p>
Public housing authorities (PHAs) have been on the front lines of the COVID-19 crisis since its beginning and have continued to serve people with extremely low incomes, who are disproportionately burdened by the pandemic’s health and economic effects. In addition to maintaining basic operations, PHAs have initiated new efforts to support residents, such as conducting regular wellness calls with older residents and those with disabilities and leveraging existing partnerships to bring food and other services on site. Some PHAs are finding new ways to engage virtually: at Westbrook Housing Authority, staff are now communicating with residents in the agency’s congregate care property via Echo Dot smart speakers. And PHAs are currently leading the way in helping their residents get vaccinated.
PHAs are well positioned to provide more than housing and were successfully doing so before the pandemic. Now they’re helping ensure equitable service delivery to people who may experience challenges accessing vaccines through existing channels. Policymakers and practitioners should recognize PHAs’ full potential and work with them to strengthen service delivery moving forward.
PHAs are leading vaccination and other service delivery efforts
Many public housing properties—which serve many older adults, people with disabilities, people of color, and, in some locations, immigrant families—have experienced high infection and mortality rates. In Minneapolis, 7.7 percent of Minneapolis Public Housing Authority (MPHA) residents who tested positive and were hospitalized passed away, compared with 1.2 percent of the city’s total population. In many cases, these outcomes resemble those of other low-income communities across the country, which have experienced the brunt of COVID-19 infections and death. Despite taking necessary precautions and offering on-site testing, many public housing authorities like MPHA have witnessed COVID-19’s devastating impact firsthand.
Faced with this situation, PHAs have stepped in to help. PHAs are well positioned to support local vaccination efforts because of their ongoing COVID-19 response activities, their relationships with the communities they serve, and their location within those communities. Since January 2021, agencies across the country have coordinated with local governments to host vaccination clinics on site. From small agencies, like the Central Falls Housing Authority in Rhode Island, to the nation’s largest agencies, such as the Chicago and DC Housing Authorities, PHAs are partnering with hospitals and clinics to bring vaccines to their properties at impressive rates. Agencies also are vaccinating their frontline staff—essential workers who often need to appear in person, including maintenance staff, social workers, and other service coordinators.
PHA-led vaccine distribution works well because PHAs know their residents, have established communications processes, and have dedicated staff to support implementation. Nonetheless, these distribution efforts have been a heavy lift for agencies already stretched thin. In Central Falls, staff went door-to-door to preregister residents before their partner agency, the Medical Reserve Corps, inoculated residents in their units. The Chicago Housing Authority partnered with the city health department to hold vaccination clinics at 44 senior properties while a mobile vaccine clinic visited seniors living in the housing authority’s family buildings. The DC Housing Authority held on-site and mobile vaccine clinics in partnership with Johns Hopkins Healthcare Systems and United Medical Center.
PHAs are spearheading equitable vaccine distribution by targeting underserved populations
Despite vaccination campaigns targeting older adults and other high-risk groups, and despite evidence of vaccine needs in overcrowded areas and among communities of color, reports indicate these populations have not been equitably served. The vaccine has been out of reach for people with limited capacity and those without family members who can help them secure appointments (which often entails accessing the internet, navigating complex registration procedures, and transporting family members to appointments). According to PBS, “The vaccine rollout [in Portland, Oregon] and elsewhere has strongly favored healthier seniors with resources… while more vulnerable older adults are overlooked.”
Without hands-on assistance, those with the greatest need—many of whom live in or qualify for subsidized housing—are left behind in COVID-19 recovery efforts. In many cases, populations served by PHAs have been unable to secure vaccine information and appointments because of difficulty with internet access, transportation, and other obstacles. By bringing vaccine opportunities on site, PHAs are removing barriers, ensuring those most in need have viable opportunities to access resources.
And because public housing tends to be in areas with high infection rates and the most vulnerable residents, vaccinating residents is reducing rates of illness and transmission in the surrounding neighborhoods. PHAs also are helping address vaccine hesitancy, leveraging their existing relationships with clients to manage vaccine concerns in a culturally competent way. PHAs have trusted staff on hand to answer questions, and many residents may feel more comfortable or inclined to receive the vaccine.
PHA’s COVID-19-related service delivery can serve as a model for future initiatives
Coronavirus Aid, Relief, and Economic Security Act funding and guidance from the US Department of Housing and Urban Development has helped solidify PHAs’ ability to cover costs related to vaccine distribution and logistics. Many PHAs have maintained strong relationships with local and state departments of health and social services, as well as other service providers, which has enabled them to act quickly and effectively on vaccine distribution. Moving forward, federal and local governments should continue to coordinate with PHAs as trusted partners and implementers, recognizing their role as liaisons with communities that too often are neglected.
Intra-agency coordination remains an important component of maximizing PHAs’ strength, as does funding for resident services initiatives. Whether from the federal, state, or local level, or from other public and private sources, resources for services allow PHAs to continue to extend their reach beyond housing. PHAs use funding for services to support ongoing health and wellness initiatives, along with education, workforce, and other programs for residents.
Having dedicated staff to develop trusting relationships with residents and manage large-scale resource distribution has proven necessary during a public health crisis. As a result, policymakers and practitioners should prioritize facilitating PHA partnerships and sustaining and expanding funding for resident services to bolster equity and address disparities moving forward.
The Urban Institute has the evidence to show what it will take to create a society where everyone has a fair shot at achieving their vision of success.
Let’s help communities build more secure, hopeful futures.
Today’s complex challenges demand smarter solutions. Urban brings decades of expertise to understanding the forces shaping people’s lives and the systems that support them. With rigorous analysis and hands-on guidance, we help leaders across the country design, test, and scale solutions that build pathways for greater opportunity.
Your support makes this possible.