
<p>Emergency workers take a resident to receive medical attention after a fire was extinguished at the Fort Lincoln Senior Citizen’s Village Apartments in Washington, DC. Photo by Bill O'Leary/The Washington Post via Getty Images.</p>
Over the past several years, devastating fires in public housing developments across the country have made headlines for displacing and injuring residents and destroying units.
Just last month, a fire in the Fort Lincoln Senior Citizen’s Village Apartments, owned by the District of Columbia Housing Authority, threatened the lives and homes of residents with limited mobility, sending five people to the hospital and 29 households to nearby hotels.
As evidenced by this and other reports, much of the nation’s public housing stock is in poor condition, creating health hazards that put older adults at serious risk. Broken boilers, mold and mildew, rodent infestations, and fires—to name a few—have damaging effects on residents of all ages, including vulnerable seniors.
To address their housing problems, public housing authorities are using a variety of financial tools to refurbish, replace, and rebuild crumbling properties. But in many cases, the available funds are inadequate. And although redevelopment promises improved living conditions, our research on previous public housing transformation efforts documents serious risks for older and frail residents.
Of particular concern, a recent US Department of Housing and Urban Development study looking at housing authorities that have financed redevelopment efforts through the Rental Assistance Demonstration (RAD) found that residents in these communities were disproportionately likely to rate their health as poor. This finding suggests that housing authorities will need to provide extra support to frail and elderly residents living in properties targeted for redevelopment.
We are not prepared to meet the increasing low-income senior population
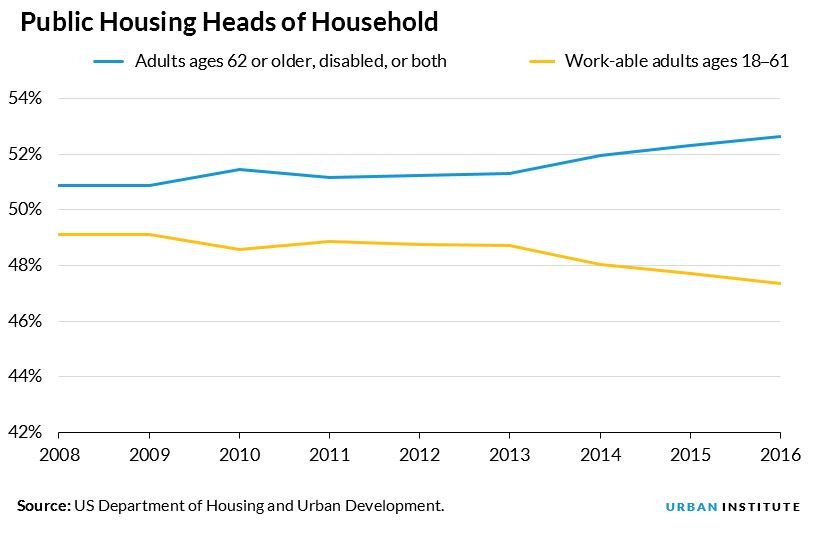
Today, more than half (53 percent) the 1.13 million households living in public housing are headed by a person who is 62 or older and/or disabled. Forty-seven percent are adults able to work.
The number of older Americans living in public housing is likely to increase (PDF) as the population of Americans older than 65 increases. In 15 years, one in three households (PDF) will be headed by a 65-year-old.
Older adults of all socioeconomic backgrounds face considerable housing-related challenges as they age. Irrespective of income, activities of daily living become more difficult, and seniors may need assistance dressing, bathing, and preparing meals for themselves.
These issues are paramount for seniors living in public housing, who overwhelmingly occupy units that have not been designed for aging in place. Less than 20 percent of all subsidized renters currently live in accessible units, and only 35 percent live in potentially modifiable units.
In some cases, seniors living in public housing may be overhoused in units that once accommodated their larger families; in others, they may struggle to secure additional assistance and affordable services.
Our earlier research on public housing transformation highlighted another risk—many older adults in these communities are raising grandchildren for a variety of reasons. That missing middle generation means there may not be an adult family member able to care for them when they grow frailer.
Existing policies are not meeting seniors’ needs
Existing policies are not adequate to meet the needs of current and future generations of seniors living in public housing.
Relocation challenges aside, there are a limited number of subsidized housing programs that serve seniors specifically and even fewer that provide services and supports for seniors aging in public housing:
- Many low-income seniors qualify for some Medicaid long-term care benefits, but the program does not include long-term care insurance, and thus, many public housing residents age in the units they have lived in for years.
- The Section 202 Supportive Housing for the Elderly program also provides housing and services for low-income seniors, but Congress has not provided new program funds since 2012.
- Within public housing, the Elderly/Disabled Service Coordinator program, now funded through the Public Housing Operating Fund, is the sole resource available to senior residents. The program funds a service coordinator at participating housing authorities, yet it isn’t able to support the increasing number of seniors aging in place. This funding is lost altogether after units convert through RAD, further limiting its scope and impact.
Seniors living in public housing will increasingly feel the negative effects of the depreciating public housing stock, and, in some case, face relocation.
Yet there are some promising practices, such as fully constructing new buildings before relocating seniors and providing comprehensive support services before, during, and after relocation. However, we need to continue building the evidence base of best practices to reduce the likelihood of bad outcomes, directly involving senior residents in these conversations.
Let’s help communities build more secure, hopeful futures.
Today’s complex challenges demand smarter solutions. Urban brings decades of expertise to understanding the forces shaping people’s lives and the systems that support them. With rigorous analysis and hands-on guidance, we help leaders across the country design, test, and scale solutions that build pathways for greater opportunity.
Your support makes this possible.