
<p>(Thanasis Zovoilis / Getty Images)</p>
Mothers have suffered tremendously during the pandemic. They have lost jobs at a higher rate than fathers and have borne the brunt of caregiving and virtual learning activities in many families. Pregnant women and new mothers have had to navigate virtual prenatal and postpartum care, and many have had more limited support from family and friends because of hospital policies and social distancing guidelines.
But with the passage of the American Rescue Plan Act, many new mothers and other birthing people can worry less about the possibility of losing their health insurance coverage. The bill contains a much-anticipated provision giving states the option, starting in April 2022, to extend pregnancy-related Medicaid/Children’s Health Insurance Program (CHIP) coverage for a year following the end of pregnancy. Currently, such coverage expires just 60 days after delivery, placing many new mothers at risk of uninsurance during a particularly critical time for mother and baby.
Extensive research evidence suggests this policy change could result in increased coverage and improved health care access and affordability among thousands of new mothers nationwide.
The potential for extension to reduce postpartum uninsurance
According to Urban Institute research, if every state adopts this new provision, approximately 123,000 uninsured mothers could become newly eligible for Medicaid/CHIP coverage during their infant’s first year. If policymakers in Florida, Georgia, and Texas alone choose to implement this provision, nearly 70,000 uninsured mothers could become newly eligible for postpartum Medicaid coverage. Thousands more covered by more expensive private plans could also benefit if they could instead retain Medicaid/CHIP, and even moms eligible for Medicaid under current policy could benefit from the certainty that their coverage would last a full year regardless of changes in income.
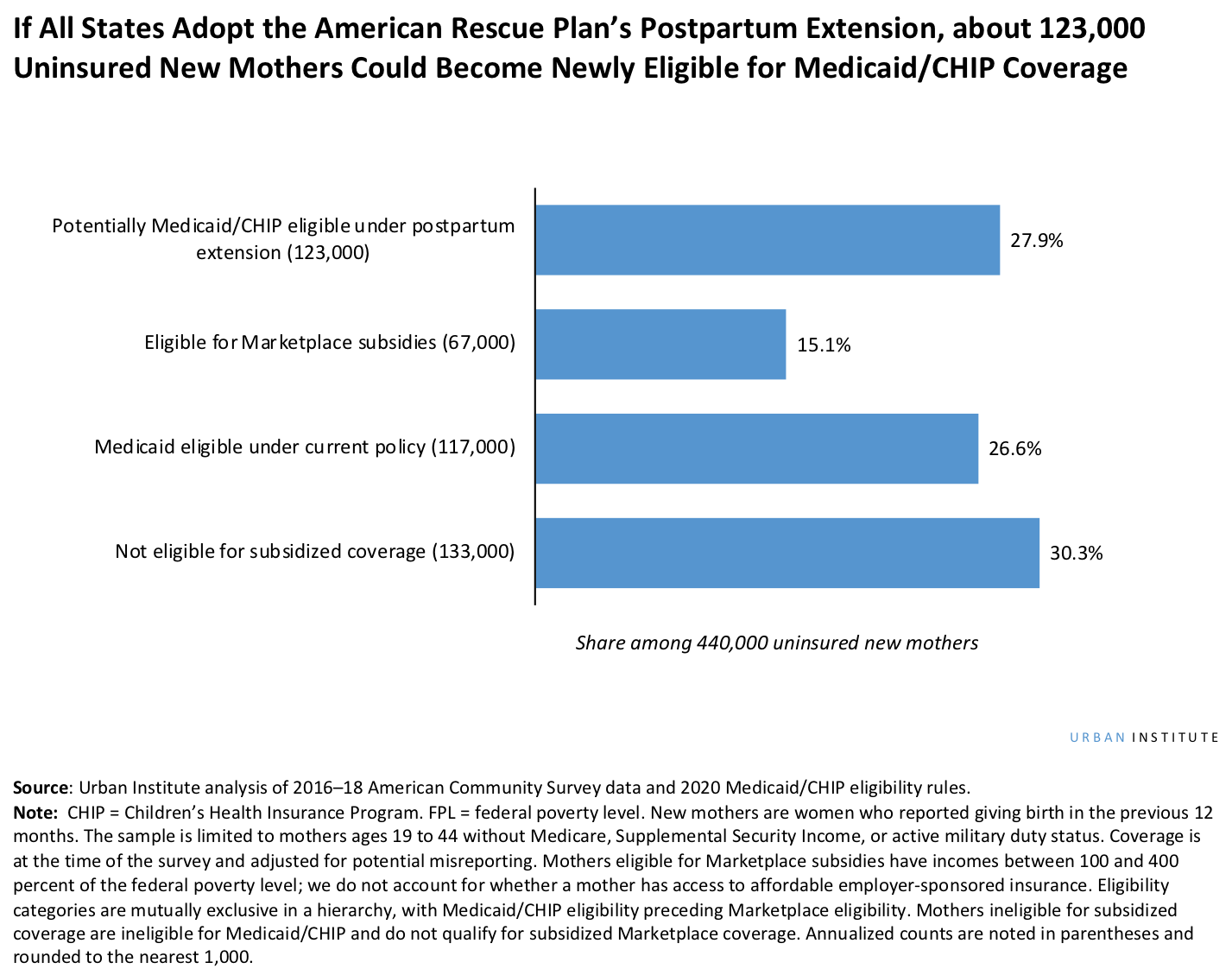
Likely improvements in health care access and affordability
Uninsured new mothers often have problems affording needed care; 23.2 percent face unmet needs for medical care, mental health care, or medications because of the cost, and 52.1 percent report being very worried about medical bills. These mothers also have substantial health needs that could benefit from consistent coverage during the postpartum period. Among mothers in 43 states who lost pregnancy-related Medicaid coverage and became uninsured, 32.3 percent were recovering from a cesarean delivery, 30.6 percent were obese, and 27.3 percent reported feeling depressed at least some of the time in the months following their delivery.
Evidence also suggests maintaining insurance coverage through a postpartum extension will likely reduce affordability concerns and improve access to care among new mothers. Following the Affordable Care Act (ACA) coverage expansions in 2014, uninsurance among new mothers declined by about 44 percent, with simultaneous declines in unmet needs for medical care and prescription medicines of 60 and 40 percent, respectively. New mothers were also more likely to have seen a general doctor, visited a mental health provider, and received a flu vaccine after 2014. In addition, continuity of coverage through the prenatal and postpartum periods has been associated with increased receipt of recommended postpartum care.
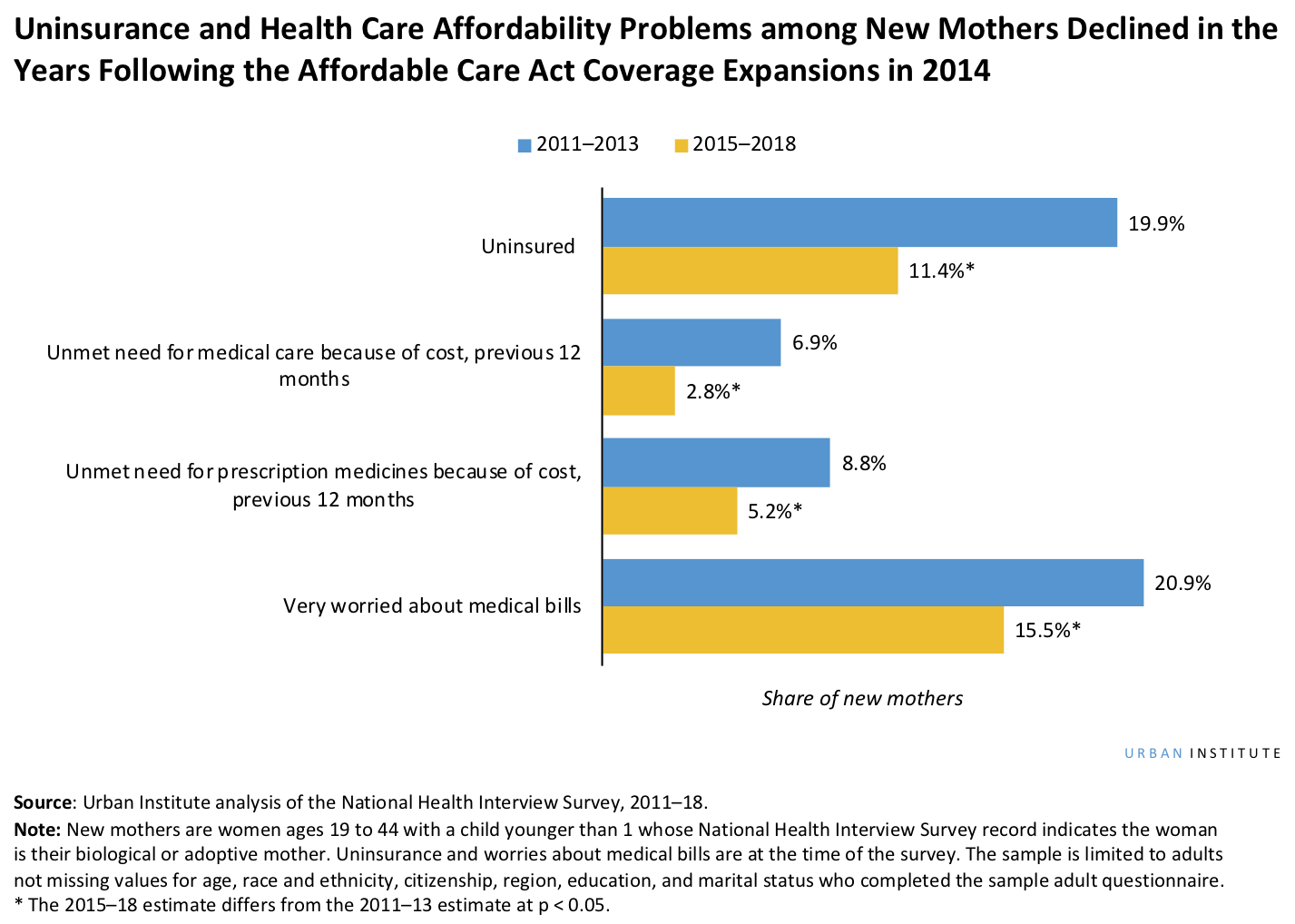
The benefits of extension will likely be more pronounced in states that have not yet adopted Medicaid expansion
Additional evidence suggests the ACA Medicaid expansion, in particular, reduced uninsurance among new mothers living in poverty in the year following delivery, reduced churning between insurance and uninsurance throughout the perinatal period, and increased utilization of postpartum outpatient visits.
Improvements in coverage, affordability, and access through a postpartum extension will therefore likely be more pronounced in states that have not expanded Medicaid under the ACA if they choose to take up the option. These states have much less generous parental eligibility and considerably higher rates of uninsurance among new mothers. But because pregnancy-related Medicaid/CHIP eligibility is more generous than that for parents in nearly all states, women in expansion states will also benefit if their states take up the option.
The effects will depend on state decisions and the effectiveness of enrollment and retention efforts
Several factors may limit the effectiveness of the postpartum extension. First, the extension is optional, so how many and which states choose to participate when the option goes into effect in April 2022 will be important. Cost to states may be a significant barrier because the law requires states contribute at their regular match rates, which range from 25 to 50 percent of costs (PDF). But, because policymakers in nearly half of states pursued extensions in recent years and several have pending waivers to implement extensions, interest appears high.
Second, more than one in four uninsured new mothers are likely already eligible for Medicaid but not enrolled, indicating that solving enrollment and retention challenges among eligible mothers will be critical. Third, about 30 percent of uninsured new mothers will likely remain ineligible for the extension or any other subsidized coverage because of their immigration status. Finally, this provision would still leave coverage gaps before pregnancy and after the first year postpartum, especially in nonexpansion states.
The provision is a win for new mothers and evidence-based policy, but there’s more work to be done
Despite these potential limitations, this provision represents the culmination of an advocacy campaign supported by a wealth of research evidence. It provides an important example of how evidence can support policy choices that will improve population health and well-being. Hundreds of thousands of mothers and, by extension, their children, could benefit if all states take advantage of the option. This provision does not, however, fully address the devastating maternal health crisis among Black women, nor the immigration restrictions that make so many Hispanic new mothers ineligible for public coverage, so a broader set of policy changes will be necessary to reduce these vast inequities and improve maternal health for all.
Let’s help communities build more secure, hopeful futures.
Today’s complex challenges demand smarter solutions. Urban brings decades of expertise to understanding the forces shaping people’s lives and the systems that support them. With rigorous analysis and hands-on guidance, we help leaders across the country design, test, and scale solutions that build pathways for greater opportunity.
Your support makes this possible.