The One Big Beautiful Bill Act (OBBBA) established new work requirements and increased the frequency of eligibility redeterminations for adults covered by the Affordable Care Act Medicaid expansion starting in January 2027. Using the Health Insurance Policy Simulation Model, we project the impacts of these two policies on expansion enrollment among adults ages 19 to 64 in 2028, a year after these policies are scheduled to be implemented. Given the flexibilities states have with respect to implementation and likely variation in their administrative approaches and capabilities, we estimate coverage changes under three potential scenarios, in which states adopt policy and implementation choices involving high, medium, and low mitigation of coverage losses among eligible adults who are meeting work requirements or exempt.
Why This Matters
Under OBBBA, applicants and enrollees must be found to be employed or participating in work-related activities, or demonstrate that they are exempt from the requirements because they are caregivers of children younger than 14 years old or disabled individuals, have special medical needs, participate in substance use treatment programs, or meet other exemption criteria. The law requires that states use information available through existing data systems to verify compliance and exemptions without requesting additional documentation from individuals where possible. Evidence from prior Medicaid demonstration waivers with work requirements found that data matching played an instrumental role in mitigating coverage losses. However, many people are still expected to lose coverage despite meeting work requirements or being exempt because they face difficulty navigating administrative processes for reporting their work activities or exemptions. Disruptions in health coverage can result in worse health, delays in obtaining health care, unmet health needs, financial burdens, and increased barriers to employment.
What We Found
- With both six-month redeterminations and work requirements, we project that a total of 4.9 and 10.1 million fewer people will be enrolled in Medicaid expansion coverage in an average month in 2028 under high and low mitigation scenarios, respectively, relative to a scenario without either of these two policies.
- This represents an enrollment decline of between 27 and 55 percent among those subject to work requirements.
- We project coverage losses of between 3.0 and 7.0 million expansion enrollees because of work requirements alone, on top of the declines in expansion enrollment of between 2.0 and 3.1 million in 2028 from six-month redeterminations.
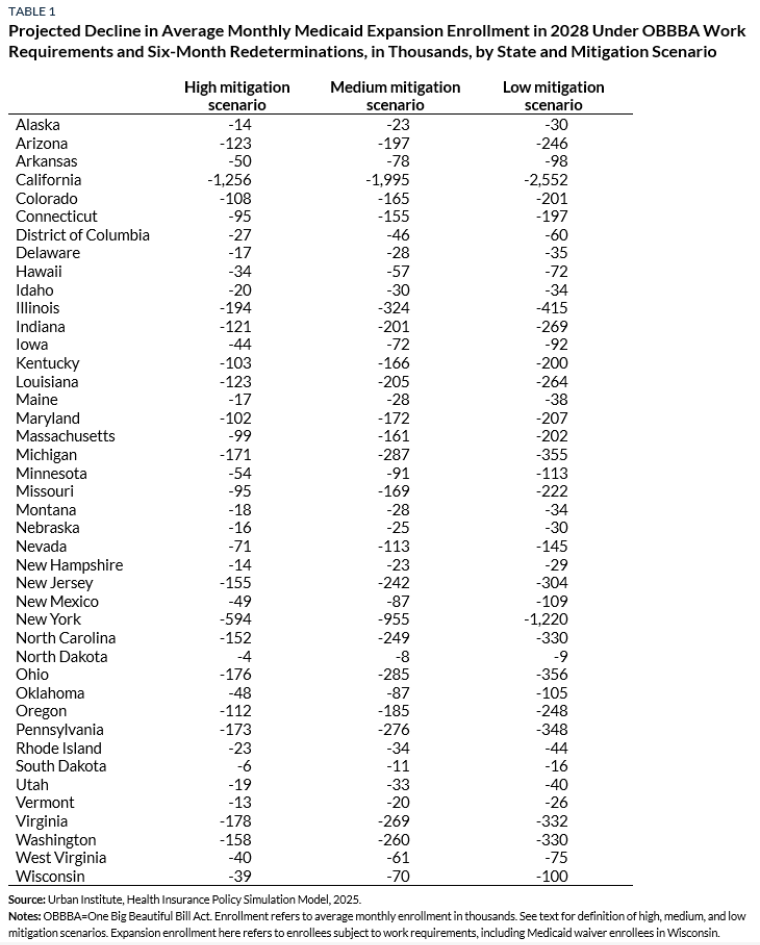
- The combined effects of these two provisions would result in lower Medicaid enrollment in every expansion state, with expansion enrollment falling by 37 to 68 percent across states in the low mitigation scenario, by 30 to 54 percent in the medium mitigation scenario, and by 18 to 33 percent in the high mitigation scenario (table 1). State-level projections assume each state makes the same policy and operational choices within each of the three mitigation scenarios. Ultimately, the actual enrollment change in each state will depend on individual state choices and capacities regarding the robustness of mitigation efforts.
- Even with robust mitigation efforts, we project that many will lose Medicaid despite potentially meeting work requirements or qualifying for an exemption. Medicaid expansion enrollment would fall by 19 to 37 percent, respectively, under high and low mitigation scenarios among people who are working, including some who are meeting the work requirement but would face challenges documenting their compliance or exemption.
- Groups at higher risk of losing Medicaid include people who are self-employed, ages 50 to 64, with a health condition affecting their ability to work, students, or caregivers for disabled family members.
Implementation choices will have a major effect on the magnitude of coverage losses, but even with robust mitigation efforts, millions of adults, many of whom are working or have health-related work limitations, are at risk of losing Medicaid.
How We Did It
We use the Urban Institute’s Health Insurance Policy Simulation Model to estimate changes in average monthly Medicaid expansion enrollment for 2028 resulting from these two policies, accounting for enrollment dynamics and potential reenrollment among people denied coverage because of work requirements. We estimate enrollment changes under three scenarios representing a range of state implementation and policy choices involving mitigation of coverage losses at redetermination and among people who are meeting work requirements or exempt:
- a high mitigation scenario, in which states minimize the number of months applicants and enrollees must comply with work requirements, maximize exemptions, and use strategies like data-matching to make it as easy as possible for people to keep their coverage without unnecessary paperwork;
- a low mitigation scenario that would impose greater levels of work effort for meeting work requirements, offer narrower exemptions, and require more efforts by applicants and enrollees to document their compliance or exemptions from work requirements;
- and a medium scenario, which would fall somewhere in between.