Highlighting the importance of public transit accessibility in promoting equitable access to care, this analysis provides new evidence on transportation barriers to health care. Using nationally representative survey data, we find that transportation barriers to health care disproportionately affect Black and Hispanic/Latinx adults and those with low incomes, disabilities, public health insurance coverage, residence in rural areas, and lack of household access to a vehicle. We also find that more than one in five adults without access to a vehicle who reported living in neighborhoods with fair or poor access to public transit forgo health care because of difficulty finding transportation.
Why this matters
Access to health care requires that affordable care is not only available but also reachable. When transportation barriers cause patients to forgo or skip health care visits, this can be detrimental to long-term health. More work is needed to understand national patterns in the role of transportation and public transit in access to medical care and, ultimately, the importance of transportation for health equity.
What we found
- Approximately 5 percent of nonelderly adults did not get needed health care in the past 12 months because of difficulty finding transportation, and this experience was more common among adults with low family incomes (i.e., below 138 percent of the federal poverty level) (14 percent), adults with disabilities (17 percent), adults with public health insurance coverage (12 percent), and adults without household access to a vehicle (13 percent).
- While 91 percent of adults reported having household access to a vehicle, this figure was substantially lower among Black adults (81 percent), adults with low family incomes (78 percent), adults with a disability (83 percent), and adults with public health insurance (79 percent) or no health insurance coverage (83 percent).
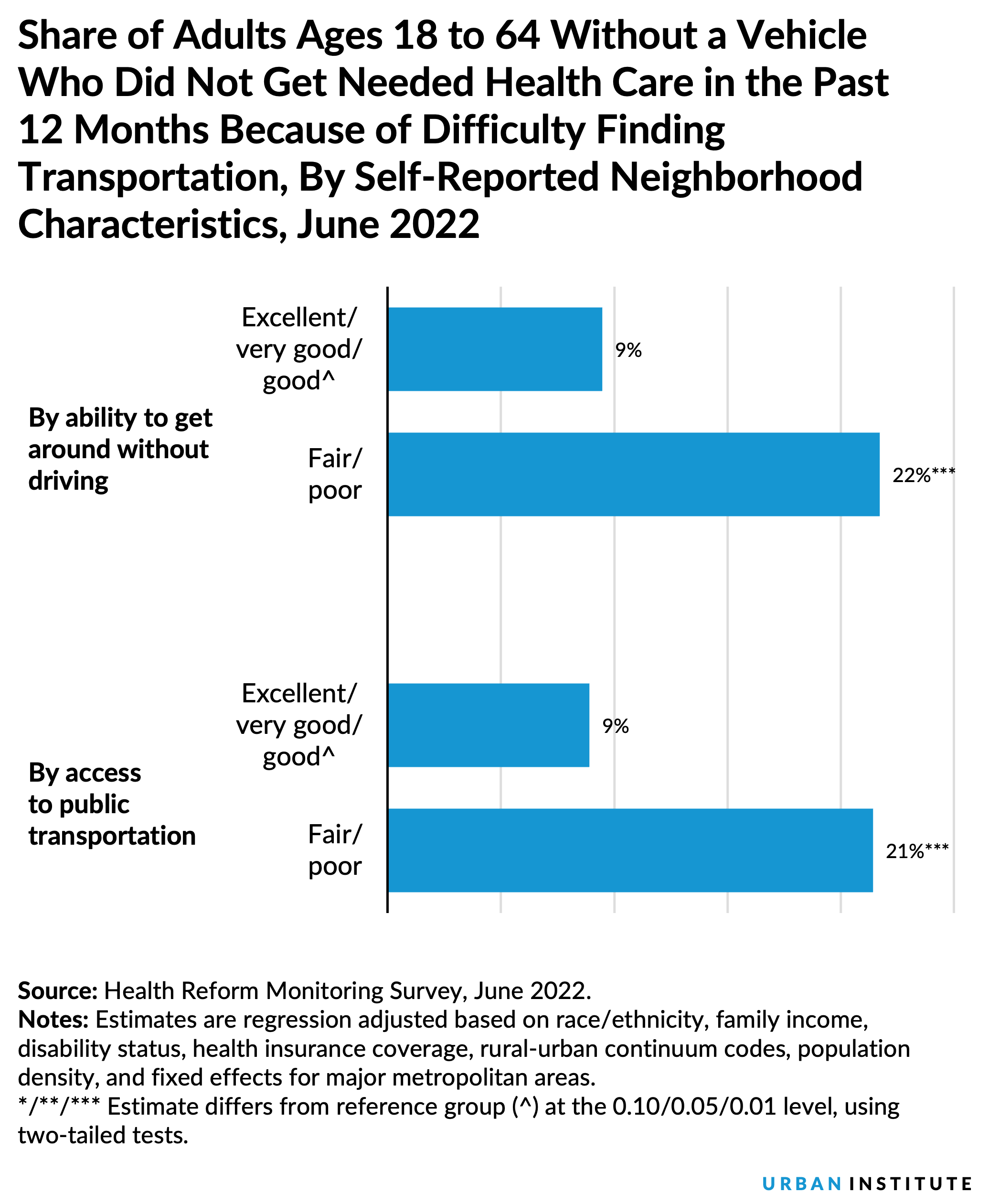
- Adults without access to a vehicle who reported living in neighborhoods with fair or poor access to public transit were significantly more likely to forgo needed health care because of difficulty finding transportation (21 percent) compared with their counterparts reporting excellent, very good, or good neighborhood access to public transit (9 percent).
- City-level transit scores from Walkscore.com, based on distance to transit stops and frequency of transit service, were less predictive of access to health care than self-reported measures of neighborhood public transportation access.
How we did it
Using June 2022 data from the Urban Institute’s Health Reform Monitoring Survey, we examine transportation barriers to health care and the association between public transit accessibility and access to care. We estimate the share of adults who had unmet health care needs or who missed or skipped health care visits in the past 12 months because of difficulties finding transportation, and how these experiences vary by race and ethnicity, family income, disability status, and other characteristics. We further assess the association between measures of access to public transit (self-reported and from WalkScore.com) and unmet health care needs.