The 2025 budget reconciliation law, the One Big Beautiful Bill Act (OBBBA), introduces significant changes to Medicaid coverage under the Affordable Care Act (ACA) expansion that are slated to be implemented beginning in January 2027. Under OBBBA, Medicaid enrollees and applicants in the expansion eligibility category will be subject to new work requirements and more frequent eligibility redeterminations. Pregnant and postpartum women are exempt from OBBBA’s work requirements and are not subject to semiannual eligibility checks because of federal continuous coverage requirements throughout pregnancy, delivery, and the postpartum period—up to 12 months after the end of pregnancy in most states. They may nonetheless face a heightened risk of disenrollment under OBBBA if state agencies are unable to promptly identify expansion enrollees who are pregnant or postpartum.
In this brief, we analyze Medicaid claims data to estimate how many pregnant and postpartum women enrolled in the Medicaid expansion category may be at risk of coverage loss under OBBBA. Drawing on existing literature, policy analysis, and interviews with Medicaid maternal health stakeholders, we also describe the operational challenges states may face in ensuring continuous coverage for pregnant and postpartum enrollees and outline potential strategies to mitigate coverage disruptions.
Why This Matters
Medicaid is a critical source of health insurance coverage for pregnant and postpartum women, financing more than 4 in 10 births in the US. While many pregnant and postpartum women qualify through pregnancy-related eligibility pathways, a notable share are enrolled through the ACA Medicaid expansion category. Successful implementation of pregnancy-related exemptions from OBBBA requirements depends on state Medicaid agencies being able to accurately identify enrollees’ pregnancy and postpartum status in a timely way and maintain their enrollment accordingly. Any gaps in coverage during pregnancy or the postpartum period could undermine access to essential care and increase the risk of adverse maternal and infant health outcomes.
Key Findings
Our analysis suggests that well over 100,000 pregnant and postpartum women are likely to be enrolled through the Medicaid expansion eligibility category in 2027 and, therefore, could be at risk of disenrollment under OBBBA’s work and redetermination requirements. We find that among enrollees with Medicaid-covered births in 2022 in expansion states, 23.8 percent had expansion coverage six months prior to their delivery, 15.6 percent had expansion coverage during the month of their delivery, and 15.9 percent had expansion coverage six months postpartum. These shares varied considerably across expansion states, ranging from less than 1 percent in Utah to 43 percent in Montana (see figure below). Enrollees in California, Kentucky, Louisiana, New York, and Pennsylvania represented nearly half of all enrollees in the expansion category during the month of delivery.
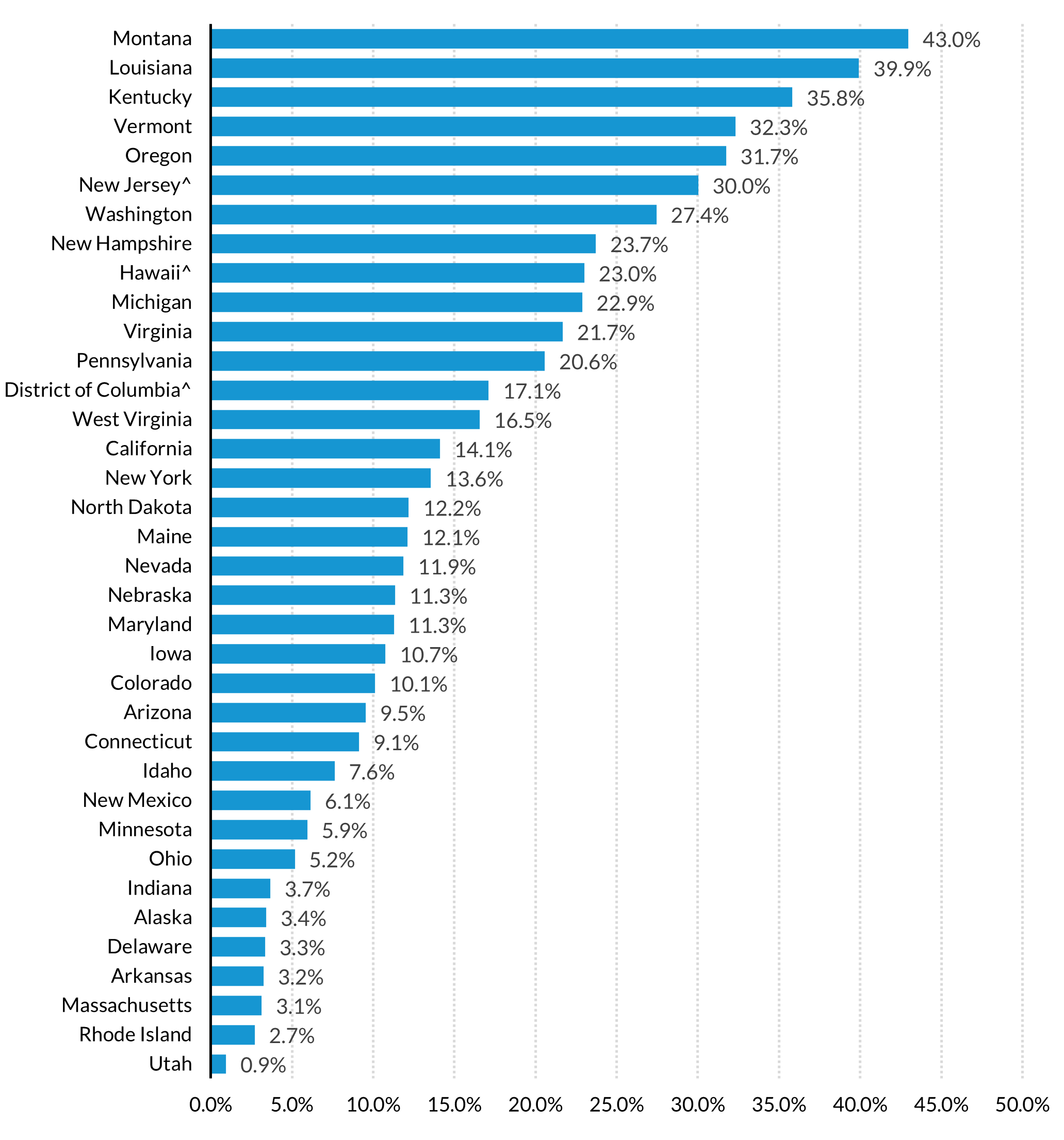
Source: Authors’ analysis of T-MSIS data in 36 expansion states (including the District of Columbia).
Notes: ACA = Affordable Care Act. Sample includes 878,214 enrollees with a Medicaid/CHIP-covered live birth in 2022. ^State has potential data quality issues; results should be interpreted with caution.
Recommendations
Historically, states have not needed to proactively identify pregnancy among expansion enrollees, which could limit their ability to automatically exempt pregnant and postpartum women from work requirements and promptly suspend semiannual redeterminations. To help ensure continuous coverage for pregnant and postpartum expansion enrollees under OBBBA, state and federal policymakers could consider the following actions and strategies:
- Leverage data more effectively and improve redeterminations. State Medicaid agencies could use claims and encounter data in a timely manner to identify enrollees who qualify for pregnancy-related exemptions, increase rates of ex parte redeterminations, and strengthen processes, such as by allowing enrollees to self-report pregnancy or postpartum status during renewal.
- Educate key stakeholders. States could provide clear guidance to enrollees, health care providers, and maternal health stakeholders about OBBBA’s changes to Medicaid eligibility, pregnant and postpartum women’s entitlement to continuous coverage, and their exemption from work requirements and semiannual redeterminations.
- Expedite federal guidance and strengthen oversight. CMS could issue guidance reminding states of their obligation to ensure continuous coverage of pregnant and postpartum enrollees and clarify the steps states must take to meet this requirement. CMS could consider requiring monthly public reporting from states to enable federal and state stakeholders to monitor enrollment and disenrollment trends under OBBBA.
How We Did It
We analyzed data from the 2021–23 T-MSIS Analytic Files to identify Medicaid enrollees with live birth deliveries in 2022 in 36 of the 37 states that had adopted Medicaid expansion as of January 2021 (one expansion state was excluded because of data quality concerns). We also reviewed relevant literature and CMS guidance and policy materials related to Medicaid pregnancy and postpartum coverage and conducted interviews with 11 key informants, including Medicaid policy experts, maternal health advocates, and state Medicaid eligibility officials.