Prior research using the Urban Institute’s Health Insurance Policy Simulation Model found that if states dropped their Affordable Care Act (ACA) Medicaid expansions in response to reduced federal funding, 15.9 million people would lose Medicaid coverage in 2026 in the 40 states and DC that adopted the expansion, with around two-thirds likely becoming uninsured and the remainder finding coverage through an employer or the Marketplaces (Buettgens 2025). Here, we extend that analysis to assess how many parents living with children would be at risk of losing Medicaid coverage under this scenario. Although uninsurance declined among parents following ACA implementation (Haley et al. 2021), federal funding cuts that lead states to roll back expansions could reverse that progress and increase parents’ uninsurance.
Elimination of the Medicaid Expansion Would Affect an Estimated 2.4 Million Parents in 2026
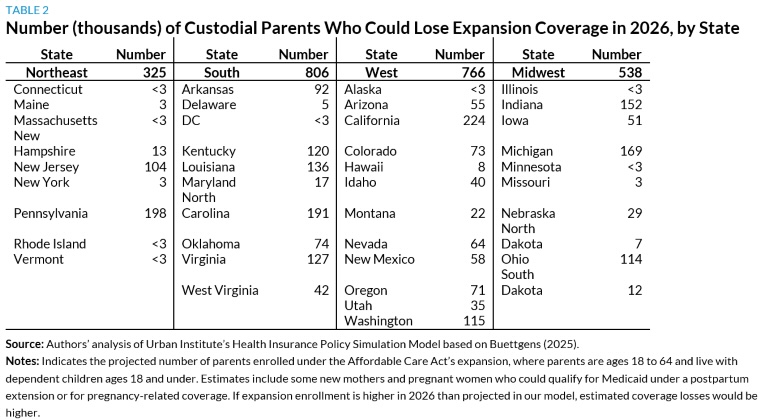
About 1.4 million mothers and 1 million fathers would have expansion coverage in 2026 and be at risk of losing Medicaid if expansions were eliminated (table 1). White parents constitute the single largest racial/ethnic group (57.5 percent or 1.4 million). At risk as well are 439,000 Hispanic parents, 402,000 Black parents, and 190,000 parents of other races/ethnicities. Almost half (48.7 percent) have incomes below the federal poverty level, and 56.0 percent live with a child under age 6. At least 100,000 parents have expansion coverage in California, Indiana, Kentucky, Louisiana, Michigan, New Jersey, North Carolina, Ohio, Pennsylvania, Virginia, and Washington, with tens of thousands covered in other states (table 2). Elimination of expansions would also cause noncustodial parents to lose coverage, and millions more parents could lose Medicaid if expansion funding cuts cause states to impose enrollment barriers or reduce eligibility for other groups of parents.

Eliminating Medicaid Expansion Would Have Adverse Implications for Parents and Children
Medicaid expansions increased adults’ treatment for chronic health issues and reduced their mortality; improved parents’ coverage, access to care, mental health, and their families’ financial well-being; and had spillover benefits for children (Guth and Ammula 2021; McMorrow et al. 2017; Hudson and Moriya 2017). Rolling back expansion coverage would likely have the opposite effects, causing many custodial and noncustodial parents to become uninsured and others to move to employer-sponsored or Marketplace plans, which would have higher cost-sharing. This would likely increase parents’ unmet health needs, stress, morbidity, and financial burdens, with their children being adversely affected because of deterioration in parental health, greater material hardships, and loss of health insurance coverage. Although eliminating ACA expansions would not target children directly, millions of children would be at risk of harm to their well-being.