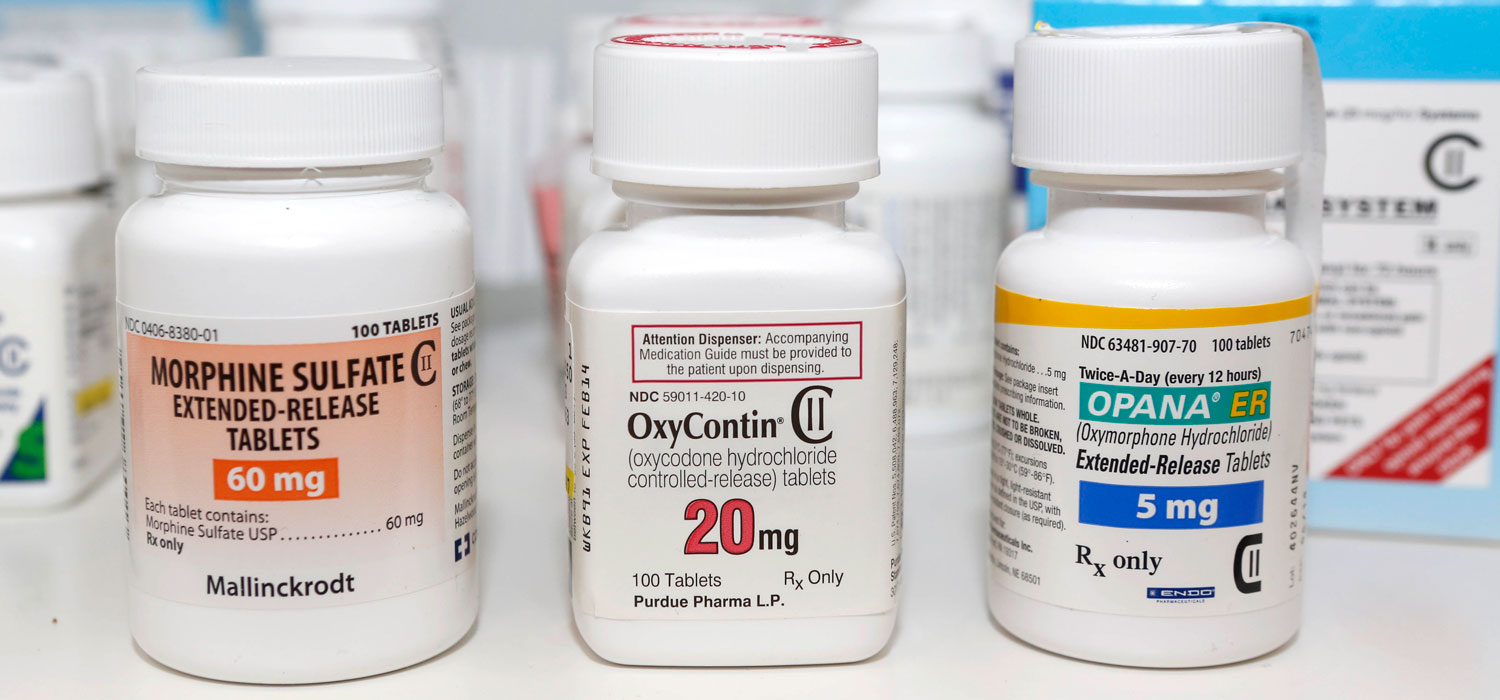
<p>In this Jan. 18, 2013 file photo, Schedule 2 narcotics: Morphine Sulfate, OxyContin and Opana are displayed for a photograph in Carmichael, Calif. Photo by Rich Pedroncelli/AP</p>
Twenty years after OxyContin first hit the market, the United States is in the midst of one of the worst drug overdose epidemics in our history. Abuse of opioid drugs and heroin continues to soar. The issue has forced its way to the top of the political agenda in critical primary states, most notably New Hampshire, where at least 385 people died of overdoses in 2015.
The epidemic is driving major increases in morbidity and mortality with huge costs to families, the social fabric of communities, and the economy. In their recent analysis of increasing death rates among middle-aged Americans, economists Anne Case and Angus Deaton called attention to “an epidemic of pain” that is fueling greater drug use, alcohol abuse, and suicides. They conclude: “if the epidemic is brought under control, its survivors may have a healthy old age. However, addictions are hard to treat and pain is hard to control, so those currently in midlife may be a lost generation.”
As we have argued before, the country should not be prepared to write off any generation as lost. But we also need to understand what really got us to this point, how we can help the many people and communities ravaged by this epidemic, and what we can do to prevent this from happening again. To date, many discussions of the opioid and heroin epidemics have focused on current trends and explanations, framing the problem as nonmedical in nature and about individual choices and behaviors.
What is less understood is how powerful commercial interests, a highly addictive drug, and weaknesses in our health care system together paved the way for this epidemic, and how better regulations and policies could have mitigated this public health tragedy.
Aggressive marketing, opioid sales, and the overdose epidemic
A comprehensive study published last January in the Annual Review of Public Health documents the parallel increases over time of opioid drug sales, opioid overdose deaths, and treatment-seeking for opioid addiction (see figure below). According to data from the National Survey on Drug Use and Health, four out of five current heroin users report that their use began with opioid drugs. Many may have turned to heroin because it is less expensive and (now) more readily available.
Rates of OPR sales, OPR-related unintentional overdose deaths, and OPR addiction treatment admissions, 1999–2010
Source: The Prescription Opioid and Heroin Crisis: A Public Health Approach to an Epidemic of Addiction
Research by public health experts, physicians, pharmacists, and journalists (including those in Canada) point to a series of events that precipitated the opioid and heroin epidemic. Chief among them are the aggressive and misleading marketing campaigns that led to widespread prescribing of these drugs by doctors and hospitals and their inclusion in private and public formularies (lists of covered drugs). The campaigns were fueled by large promotion budgets, strategic use of prescriber profiling data, direct marketing to physicians by pharmaceutical sales reps, and lucrative incentives to those reps, along with free starter coupons for patients.
Increases in opioid prescriptions for long-term use have been traced to a 1986 paper claiming that the drugs could be used safely over a long period, despite very limited scientific evidence for this change in medical practice. The paper was widely cited to promote greater use of opioids in managing chronic non-cancer pain. It was based on 38 patients.
The sharpest increases in opioid use began in 1996, exactly one year after Purdue Pharma introduced OxyContin, an extended release form of oxycodone. Purdue Pharma’s activities culminated in a policy decision to make pain the “5th Vital Sign” to raise awareness about identifying and treating pain in clinical settings, along with the help of smiley faces for pain rating scales. Many groups and organizations were on board: the American Pain Society, the American Academy of Pain Medicine, the Federation of State Medical Boards, The Joint Commission (which accredits hospitals), as well as pain patient groups. But there was no central coordinating entity paying attention to the effects of these changes on community or population health, or to possible unintended consequences.
Need for better regulation, evidence-based policies, and public health surveillance
Among the many factors that contributed to the two-decade rise in opioid use in the United States, it is clear that policy decisions and failures have played a role. Especially for drugs with a high potential for addiction and abuse, we need much stronger oversight governing how clinical use, real-world use, and addiction risks are studied and represented when first introduced to the market.
Stronger regulatory policies governing how these drugs are marketed, advertised, and sold are also critical. Many weaknesses in our current system allowed the opioid epidemic to spread. We need an active surveillance system for adverse drug events, one that prescribers have ready access to; a robust national prescription drug monitoring program, along with early warning systems for detecting problems with prescribing practices or addiction; and solid plans for addressing a public health crisis at the very earliest signs of an epidemic, along with support for addiction treatment.
Finally, with so many government and non-government entities involved in developing, testing, manufacturing, regulating, marketing, distributing, prescribing, and dispensing these powerful drugs, we need better mechanisms for holding both private industry and public-sector agencies accountable. The American public deserves no less.
In the case of opioids, investigations by the Justice Department, the Food and Drug Administration, and the Senate Finance Committee were too late to save lives. This epidemic is a powerful reminder that we need to base our public policies on strong research evidence.
“Overstated or unsubstantiated findings are not helpful for translating evidence into effective policy, and contribute to public, policymaker and media perceptions (often accurate) of unreliable, flip-flopping research findings,” Ross Koppel and Spencer Jones recently argued in Health Affairs. “Health care research must be based on the strongest feasible designs, and not on protocols that affirm our biases, support hidden funding sources, or obscure wise policy choices.”
Fortunately, some efforts are underway to identify best approaches for containing the epidemic, preventing future overdoses, revisiting policies that may not be helpful, and formulating new ones that are. But a critical lesson is that policies do matter, and the social and economic costs of getting them wrong can be very high.
Let’s build a future where everyone, everywhere has the opportunity and power to thrive
Urban is more determined than ever to partner with changemakers to unlock opportunities that give people across the country a fair shot at reaching their fullest potential. Invest in Urban to power this type of work.
